Understanding bereavement: Grief support and finding help in Australia
Learn about bereavement support in Australia, including services, counselling, and compassionate guidance. Contact Sensible Care for trusted support.
Author: Sensible Care

Bereavement refers to the period after you experience a loss. When grief disrupts work, parenting, or daily care, there are many supports you can use in Australia. Start with the right support level: crisis lines for safety, grief services for loss support, and your GP for ongoing care. Aged care providers support families with clear communication, respectful end-of-life care, and referrals for ongoing bereavement support.
Even after someone you love dies, you still need to function, make decisions, and get through each day. You may also face sleep problems, low appetite, brain fog, and sudden waves of emotion.
This period after losing someone is called bereavement.
Australia offers many forms of bereavement support to anyone going through this difficult time. Bereavement support provides practical guidance and emotional care, so you don't carry the loss alone.
It helps you connect to the right services, at the right time, based on what you need now.
This guide explains what bereavement means, how grief works, and what support services you can use in Australia. It also covers healthy coping strategies and warning signs that call for professional help.
What is bereavement, and how does it work?
Bereavement is the period a person goes through after someone close to them dies.
It doesn't only affect your emotions and thoughts, but also the challenges you face every day. The process unfolds as you handle practical tasks and adapt to daily life, step by step.
You often switch between getting things done and feeling the impact of the loss. One day you cope well, and the next day, a song, photo, or date hits you hard.
Your bereavement experience depends on who you lost, how they died, and who supports you. An expected death can leave you exhausted, while a sudden death is shocking.
Grief rarely follows "neat stages." You move back and forth as you adjust to new roles, new routines, and new meaning.
What are common bereavement reactions?
Bereavement can show up everywhere, not just in your feelings. Your body, your mind, and your relationships can all shift at once, which can feel confusing.
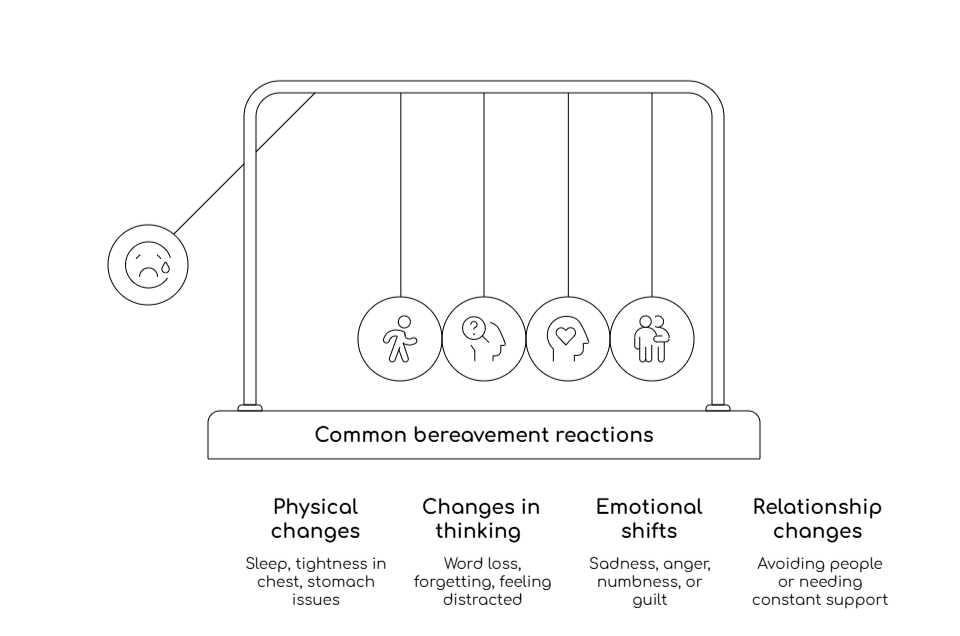
Common reactions include:
- Physical changes: Trouble falling or staying asleep, tightness in your chest, an upset stomach, headaches, low appetite, and feeling exhausted by small tasks.
- Changes in thinking: Losing words, forgetting simple things, replaying moments you cannot stop thinking about, or feeling "foggy" and distracted.
- Emotional shifts: Moving between sadness, anger, guilt, numbness, relief, and even brief moments of peace, sometimes within the same hour.
- Relationship changes: Avoiding people because talking feels too hard, needing someone close because being alone feels overwhelming, or feeling out of step with how others grieve.
Which bereavement support services are available in Australia?
There are several proven support pathways in Australia. Start with the level of help that can support how you feel today.
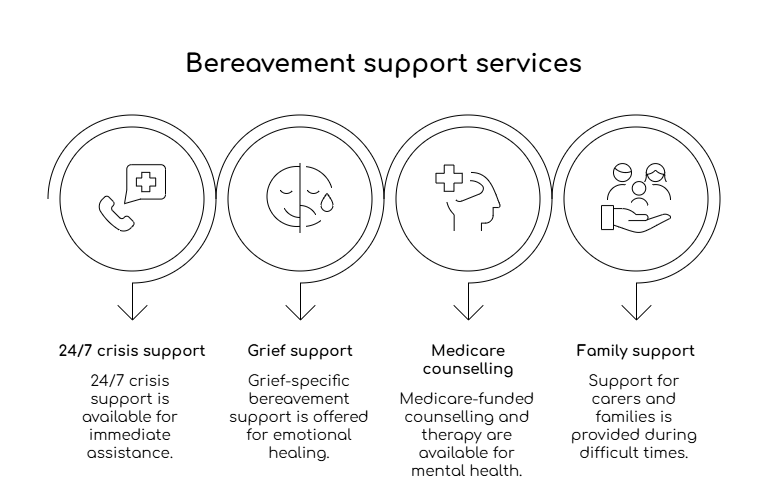
These pathways include:
- 24/7 crisis support
- Grief-specific bereavement support
- Medicare-funded counselling and therapy
- Support for carers and families
24/7 crisis support
If you feel unsafe, act fast and use emergency support. Call 000 if someone's life is in danger.
- Lifeline (24/7): 13 11 14 – crisis support by phone
- Suicide Call Back Service (24/7): 1300 659 467 – for people feeling suicidal, worried about someone, or bereaved by suicide
- 13YARN (24/7): 13 92 76 – for Aboriginal and Torres Strait Islander crisis support
- Beyond Blue (24/7): 1300 22 4636 – for anxiety, depression, and suicide prevention support
- Kids Helpline (24/7): 1800 551 800 – for young people aged 5 to 25
These services can also help you find ongoing supports in your area.
Grief-specific bereavement support
Grief-focused services help you process what you are going through in a structured, compassionate way.
Use these when you want support that directly targets grief and loss:
- Griefline (now part of SANE Australia): 1300 845 745 – free national helpline (typically 8 am–8 pm, 7 days a week) plus online forums and resources
- Grief Australia (Australian Centre for Grief and Bereavement) Freecall: 1800 642 066 – information, resources, and bereavement support services
These organisations may also help you find local support groups, online programs, or specialist bereavement services.
Medicare-funded counselling and therapy
You can use Medicare-funded mental health care when grief causes significant distress. It also applies to when your ability to work, study, care, or function day to day is disrupted.
If you choose this option, your GP can:
- Talk to you about how you are coping
- Create a Mental Health Treatment Plan, if appropriate
- Refer you to a psychologist, social worker, or other mental health professional
Under Better Access, eligible people can claim Medicare rebates. This can apply to 10 individual and 10 group mental health sessions per calendar year. But they must have the right referral and plan.
Ask your GP what applies in your situation, and whether other low-cost or free options are available in your area.
Support for carers and families
Carers often carry grief while also managing exhaustion, changing roles, and practical responsibilities.
Support is available through:
- Carer Gateway: 1800 422 737 – a national service that connects carers with counselling, coaching, and practical help.
- Local community health centres, palliative care services, and bereavement services. These services can offer counselling, groups, and practical advice.
If you feel unsure which service to choose, talk to your GP, a social worker, or a helpline for guidance and local links.
What healthy coping strategies help during bereavement?
You cope best when you support your body, mind, and relationships. Think of these strategies as small, repeatable steps you use over weeks and months, not one‑off fixes.
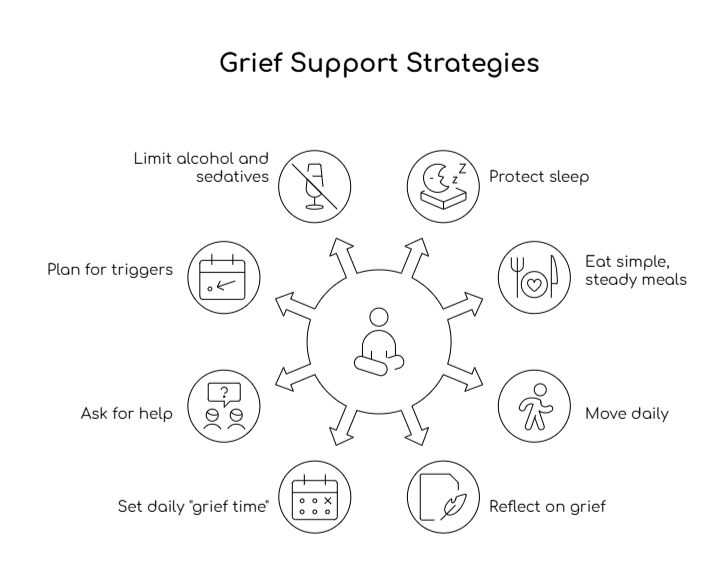
Helpful strategies can include:
- Protecting sleep: Go to bed at roughly the same time each night, reduce late caffeine, and use a short wind‑down routine before bed.
- Eating simple, steady meals: Aim for basic meals with some protein, fruit or vegetables, and water, even when your appetite is low.
- Moving your body daily: Take a 10‑minute walk, stretch, or do gentle strength work to release stress and support mood.
- Reflecting on your grief: Write a few sentences each day about what you lost, what you miss, and what you fear or hope for.
- Setting a daily "grief time": Create one daily time block, such as 20 minutes, for photos, tears, or journaling, so grief has space without taking the whole day.
- Asking for specific help: Request concrete support such as meals on Tuesdays, school pickup on Fridays, or one phone call each evening.
- Planning for triggers: Plan extra support around anniversaries, birthdays, holidays, hospital or facility dates, and other reminders.
- Limiting alcohol and sedatives: These can disrupt sleep, increase low mood, and make coping harder the next day.
These steps don't remove grief, but they can make the days more manageable and help your body and mind recover over time.
When is it time to seek professional bereavement help?
Seek professional help when grief blocks your basic functioning, or when your safety feels at risk.
Get urgent support if you:
- Have thoughts of self‑harm or suicide
- Feel out of control or unable to keep yourself safe
- Feel you may harm yourself or someone else
In these situations, call Lifeline 13 11 14, Suicide Call Back Service 1300 659 467, or 000 in an emergency.
Seek clinical support from your GP or a mental health professional when, over several weeks, you notice patterns such as:
- You can't work, parent, or complete daily care tasks without breaking down.
- You avoid all reminders of the person who died, or you feel stuck in constant searching, replaying, and rumination.
- You rely on alcohol, drugs, or risky behaviour to numb the pain.
- You feel persistent hopelessness, intense guilt, or unbearable loneliness.
- Your grief stays very intense and disabling long after what most people around you would expect.
Clinicians may also screen for Prolonged Grief Disorder. This is a condition where severe grief persists and interferes with daily life for a long time. In adults, diagnosis requires that at least 12 months have passed since the death; in children and adolescents, at least six months.
If you're unsure whether what you feel is "normal," it is always appropriate to ask your GP or a counsellor.
How do aged care providers support families through bereavement?
Aged care teams support you with practical guidance and clear communication before and after a death. Of course, they also provide referral pathways.
Aged care quality expectations include recognising emotional needs and involving families in decisions. This also includes preserving dignity during end‑of‑life care.
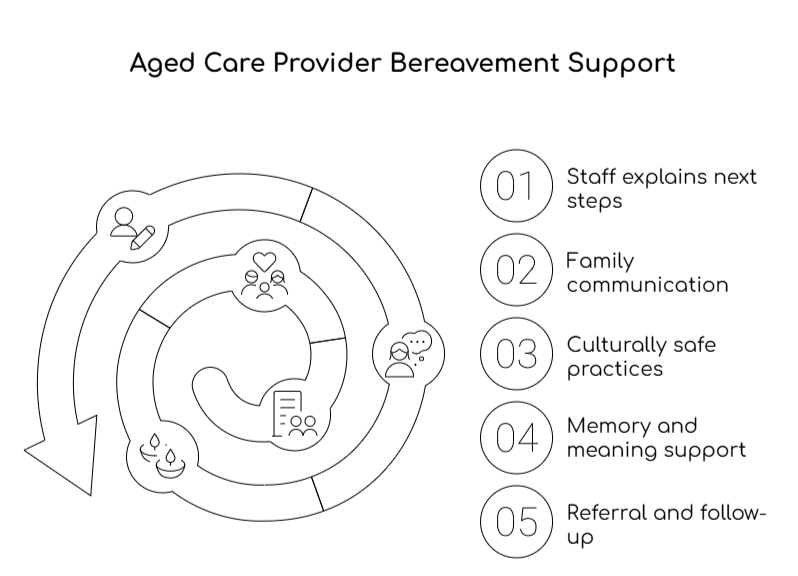
You can expect support that includes:
- Clear next steps: Staff explain what happens after death, including belongings, paperwork, and key contacts.
- Family communication: You get one consistent point of contact, plus honest updates and time to ask questions.
- Culturally safe practices: Staff respect rituals, language needs, and family decision-making structures.
- Memory and meaning support: You receive options for viewing, a quiet space, condolence practices, or memorial moments.
- Referral and follow-up: Staff connect you with bereavement services, your GP, and local supports, and they check in after the death.
If you want support that stays coordinated, contact Sensible Care and ask for bereavement guidance and referrals.
FAQ
Can bereavement turn into Prolonged Grief Disorder?
Yes. Prolonged Grief Disorder describes grief that remains intense, disabling, and persistent beyond typical cultural expectations. Diagnostic criteria require that the death occurred at least 12 months ago for adults, or six months ago for children and adolescents.
Can you get Medicare help for bereavement counselling?
Yes, if grief is causing significant distress or functional problems, and you meet the eligibility criteria. Medicare rebates may apply through Better Access. Eligible people can access rebates for up to 10 individual and 10 group therapy services per calendar year.
How do you support a child through bereavement?
Use simple, direct words like "died" instead of vague terms, and answer questions honestly at their level. Keep routines as steady as possible, name feelings you see, and offer extra comfort and predictability. If your child struggles, seek support from school wellbeing staff, your GP, child‑focused grief services, and Kids Helpline (1800 551 800).
What should you do on anniversaries?
Plan the day before it arrives. Choose one ritual, one support person, and one recovery activity, like a walk or an early night. Tell your workplace and family what you need, in one clear sentence.
Let Sensible Care help you get through this difficult time
Bereavement support helps you stay steadier after a loss and face the days ahead with less overwhelm. You build more stability through simple routines, clear support, and honest conversations.
Reach out when grief disrupts sleep, work, caring responsibilities, or safety. Use crisis services for emergencies, and talk to your GP and grief services for ongoing support.
When you want practical guidance and compassionate follow‑up, contact Sensible Care.
As an aged care and support‑at‑home provider, Sensible Care supports you. We will help you with clear next steps after a death, compassionate check‑ins, and help coordinate what happens next.
Sensible Care can organise in‑home support and link you with bereavement counselling. We can also work with your GP and family, so support stays consistent and personal.
Contact us if you want to know more.
Take the Next Step in Care
Download our Info Kit or speak to one of our friendly team members today.
Need Help Getting Started?
Reach out on your terms, pick a time that suits you and let’s talk about how we can help.
.webp)
.svg)


