What is dignity of risk?
Dignity of risk is the right to make your own choices, even risky ones. Learn what it means in aged care and NDIS support, and why it matters.
Author: Sensible Care

Dignity of risk is the right to make your own choices, even when those choices involve some risk. It applies to older Australians in aged care and people with disabilities on the NDIS. The Aged Care Act 2024 and the NDIS Practice Standards both protect this right. This approach respects the person's independence, identity, and quality of life.
Dignity of risk means you have the right to make your own choices and take reasonable risks, even when those choices might lead to harm. It applies to older Australians in aged care and people with disabilities receiving NDIS support.
The idea is simple. Making your own choices is part of being human and shapes who you are. When care providers remove every risk in the name of safety, they also take away your independence and sense of self.
Dignity of risk definition: What does it mean?
Dignity of risk is the idea that you have the right to live the life you choose, even when your choices carry some risk.
It's not a free pass for careless behaviour. It's about recognising that the right to make your own decisions is part of being human.
This principle is recognised by the Aged Care Quality and Safety Commission. The same idea applies in residential aged care, home care, and NDIS support.
The term was first used by American chaplain and disability advocate Robert Perske in 1972. He argued that protecting people from every risk strips them of their dignity and stops them from becoming who they could be.
Why dignity of risk matters in aged care and disability support
Older adults, who are supported to take reasonable risks, may gain measurable benefits, including:
- Increased social interaction
- Independence
- Hope
- Empowerment
- Self-esteem
- Self-determination
Removing all risk doesn't protect people — it harms them. Over-protection in care settings is a known cause of:
- Social isolation
- Physical decline
- Cognitive decline
- Loss of purpose
Research published in PMC confirms that overly cautious care can harm a resident's wellbeing. The goal is not to remove risk but to manage it in a way that respects each person's right to live meaningfully.
The cost of over-protection
Over-protection happens when a provider limits someone's choices for the wrong reasons. Not because the risk is unreasonable, but because of worry about liability or discomfort. Common examples include:
- Keeping a resident in their room to prevent falls
- Stopping someone from joining community activities because they might wander
- Taking away a walking frame and insisting on a wheelchair
- Cancelling a resident's daily walk because the path is wet
- Choosing soft foods for a person who prefers a normal diet
These restrictions create what researchers call "dignity violations." That's when safety measures become their own source of harm.
A person denied the freedom to move loses physical function. A person shut out of social activities feels isolated and grieves the loss.
What "safe enough" looks like
The idea of "safe enough" reframes what good care looks like. Providers should ask, "Which risks are worth supporting?" — not "How do we prevent all harm?"
A person who chooses to walk without a frame may fall. A person who chooses to eat food with a particular texture may cough. These outcomes are possible. But they must be weighed against the dignity, independence, and quality of life that come from respecting the person's choice.
Dignity of risk in aged care: what the law requires
Dignity of risk is built into Australian law. The Aged Care Act 2024 created a Statement of Rights for older people. It recognises the right to make decisions about your own life, including risky ones.
The strengthened Aged Care Quality Standards started on 1 November 2025. They require aged care providers to recognise and respect each person's unique:
- Identity
- Culture
- Social connections
- Wellbeing
- Needs
Dignity of risk is clearly built in throughout, particularly in Standard 1 (The Individual).
Providers now have to show that the care they deliver matches each resident's rights. They prove this through their documentation, policies, and day-to-day practice. This is a legal duty, not a guideline.
Dignity of risk in the NDIS: what providers must do
For disability support, the NDIS Practice Standards have their own definition. They describe dignity of risk as "the right of the individual to choose to take some risk in engaging in life experiences."
Outcome 1.4 (Independence and informed choice) is the main audit point. This is where registered NDIS providers have to show how they support participant autonomy and dignity of risk.
The NDIS Practice Standards require registered providers to:
- Respect each participant's right to make risky decisions
- Explain risks and consequences in a way the participant understands
- Help participants make informed decisions using supported decision-making
- Keep records of participant choices and related risks (such as plans and risk assessments)
- Continue providing support when a participant makes a dignity-of-risk choice
- Only use restrictive measures when the law allows

Dignity of risk vs duty of care: What is the difference?
Dignity of risk and duty of care aren't opposites. Duty of care is the legal duty to take reasonable steps to prevent foreseeable harm. Dignity of risk changes what that duty looks like in practice.
Under a dignity of risk approach, duty of care doesn't mean protecting someone from every possible harm. It means three things:
- The person understands the risks.
- They have access to reasonable safeguards.
- They've genuinely agreed to go ahead.
Once that process is followed and documented in good faith, the provider has likely met their legal duty. This holds true even if something goes wrong.
Providers should only override someone's choice in rare cases. These include an immediate threat to life or serious harm, or when the law requires it (for example, a court order or an authorised decision-maker). In every other situation, the person's informed choice should be respected.
Where providers go wrong
Providers often fail dignity of risk obligations by treating staff discomfort as a real safety risk. A care worker's anxiety isn't the same as an assessed, documented risk.
When providers limit activities based on staff anxiety alone, they're not exercising duty of care. They're putting staff preferences ahead of resident rights.
Guidance from The Council on Quality and Leadership (CQL) makes the same point. Teams need to tell the difference between real safety concerns and staff anxiety. Restrictions driven by fear, not assessed risk, go against dignity of risk principles.
Dignity of risk examples: what this looks like in practice
Five common dignity of risk examples come up across aged care and disability support settings.
Worked example: informed choice about food texture
Margaret is 82 and lives at home with support. Her speech pathologist recommends minced and moist food for mild dysphagia. Margaret refuses. Family meals are central to her identity, and she insists on eating normal food.
Her provider explains the aspiration risk in plain language. The care plan records Margaret's choice, the risk discussion, and the agreed safeguards. These include eating slowly, sitting upright, and having a carer present at meals.
Margaret's choice is respected. Her provider has met their duty of care through informed consent, not by overriding her decision.
Worked example: community access and wandering risk
David is 78 and has mild to moderate dementia. He's walked to his local café every morning for 20 years. His family worries that he might get lost.
His care team assesses his capacity for this specific decision. He can describe the route, recognise landmarks, and use his phone.
They fit him with a GPS safety device and give the café his contact details. The plan records his informed consent and his family's involvement.
David keeps his morning walks. His dignity is preserved, and his risk is managed rather than removed.
How to apply dignity of risk in practice: a step-by-step framework
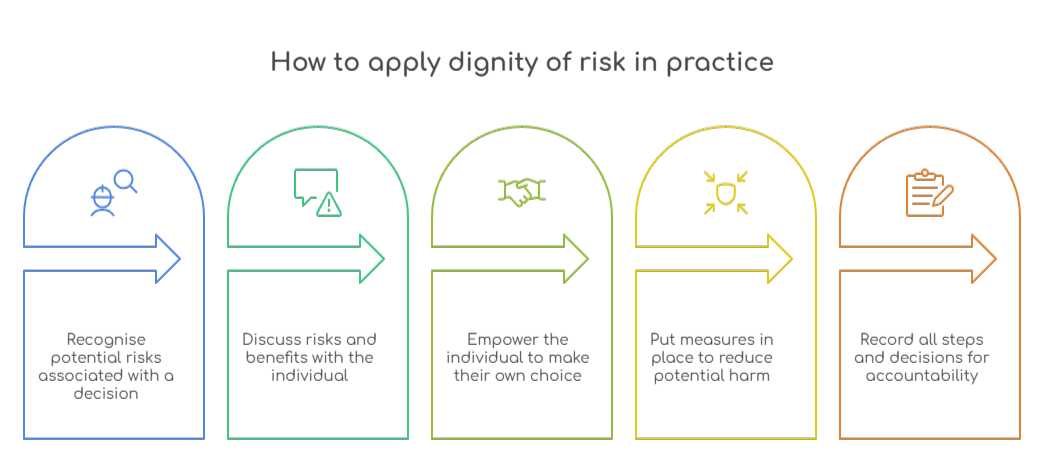
Use dignity of risk in practice by following a five-step process:
Step 1: Identify the risk
Identify the specific risk, not a vague concern, but a defined potential harm. Is the risk a fall? An aspiration event? Becoming lost? Getting sunburnt?
The more precisely the risk is identified, the easier it is to communicate clearly and manage the actual concern.
Step 2: Communicate clearly
Explain the risk to the person in language they can understand. Avoid clinical jargon. Use short sentences.
Check that the person has understood. Ask them to explain the risk back to you in their own words if helpful.
Step 3: Support the decision
Supported decision-making is the main approach in both the Aged Care Act 2024 and the NDIS Practice Standards. It means helping the person explore their options, understand the consequences, and make their own choice. It doesn't mean making the decision for them or pushing them toward the "safe" option.
Step 4: Put reasonable mitigation in place
Agree on practical ways to reduce harm without removing the choice. This can include a GPS device, a carer present at mealtimes, or a handrail on the garden path. These safeguards respect the person's independence while lowering the risk of serious harm.
Step 5: Document everything
Accurate records protect both the person and the provider. Write down the risk you identified, the information you shared, the person's informed choice, and any safeguards you agreed on. This record shows you acted in good faith. It also strengthens your defence against negligence claims if something goes wrong.
Dignity of risk for people with cognitive impairment and dementia
A person with dementia or cognitive impairment still has the right to make decisions about their own life. A diagnosis doesn't automatically take that right away.
Capacity is assessed for each decision, not assumed to be missing because of the diagnosis.
Someone with moderate dementia may not be able to make complex financial decisions. But they can still choose what to eat, who to spend time with, or whether to go for a walk.
Supported decision-making helps people with cognitive impairment make real choices. Taking away that chance damages their dignity rather than protecting them.
When assessing capacity for a specific decision, ask these questions:
- Does the person understand the information?
- Can they hold onto it long enough to decide?
- Can they weigh up the options?
- Can they communicate their decision in any way?
Dignity of risk legislation in Australia: a summary
Australian dignity of risk legislation spans both federal aged care law and NDIS regulation.
The Aged Care Act 2024 is the government's main response to the Royal Commission. It puts older people's rights at the centre, including their right to make risky choices.
How person-centred care respects client choices
Person-centred care builds support around the individual. This includes their identity, history, preferences, and goals. It doesn't build care around the provider's routines. Dignity of risk is part of this approach.
It starts with a simple question: what matters to this person? The answer shapes everything that follows, from meal times to activities to how risk is discussed. The provider's job is to support the person's choices, not make decisions for them.
This approach respects client choices in three ways:
- It treats the person as the expert on their own life.
- It helps the person weigh options without pushing them toward the "safe" answer.
- It records the person's wishes, including risky choices, as part of the care plan.
Person-centred care doesn't ignore clinical judgement. A physiotherapist still assesses falls risk. A dietitian still recommends safe textures. But these are offered as information to guide the person's choice, not as orders to override it.
Living well, your way
Dignity of risk is about respect. It recognises that older people and people with disability have the right to make their own choices, just like anyone else. Some of those choices will involve risk. That's part of being human.
At Sensible Care, we believe you should be in charge of your own life. Our team works with you to understand what matters most, talk through any risks, and build a care plan that fits the way you want to live.
Our services cover a wide range of needs. This includes personal care, domestic help, transport, social support, nursing, and allied health.
Book a free initial consultation by phone or schedule a callback to get started.
Take the Next Step in Care
Download our Info Kit or speak to one of our friendly team members today.
Need Help Getting Started?
Reach out on your terms, pick a time that suits you and let’s talk about how we can help.
.webp)
.svg)


