Stages of dementia: What to expect and how to plan care
Learn about the 7 stages of dementia, what symptoms to expect at each stage, and how to plan care for your loved one at every step of the journey.
Author: Sensible Care

Dementia progresses through stages, from early memory changes to full dependence on others for care. The two most common models are the three-stage model (early, middle, late) or the seven-stage Global Deterioration Scale (GDS). How quickly someone moves through the stages depends on the type of dementia, age at diagnosis, and overall health. Dementia cannot be reversed, but healthy lifestyle choices can lower the risk.
Dementia moves through stages. It starts with early, subtle cognitive or behavioural changes. It then progresses to severe mental and physical decline that needs full-time support.
Knowing each stage helps you plan the right care at the right time, so your loved one always has the support they need.
This article covers the two most common frameworks used to describe dementia stages.
The first divides dementia into three broad stages: early (mild), middle (moderate), and late (severe).
The second is the Global Deterioration Scale (GDS). It includes seven stages and is widely used by health professionals for clinical assessment and care planning.
Read on to find out more about the stages of dementia.
What is dementia?
Dementia is a group of conditions that affect memory, thinking, and the ability to manage daily life. It is caused by damage to brain cells from diseases such as:
- Alzheimer's disease
- Vascular dementia
- Lewy body dementia
- Frontotemporal dementia
Dementia is not a normal part of ageing. Most older Australians do not develop it, though the risk increases significantly with age.
In February 2026, an estimated 446,500 Australians were living with dementia. That figure is projected to reach over one million by 2065. Dementia is now Australia's leading cause of death, accounting for 9.4% of all deaths in 2024.
How many stages of dementia are there?
Dementia is most often described using either three stages or seven stages, depending on the purpose.
The three-stage model (early, middle, late) is used for everyday care planning and family communication.
The seven-stage GDS model is used by doctors and nurses to assess cognitive decline in clinical settings.
Both models describe the same overall disease trajectory. The seven-stage model provides more detail. This includes pre-dementia changes that the three-stage model does not cover.
The 3 stages of dementia
The three-stage model describes dementia as early, middle, and late. Each stage reflects a different level of mental and physical decline and a different level of care needed.
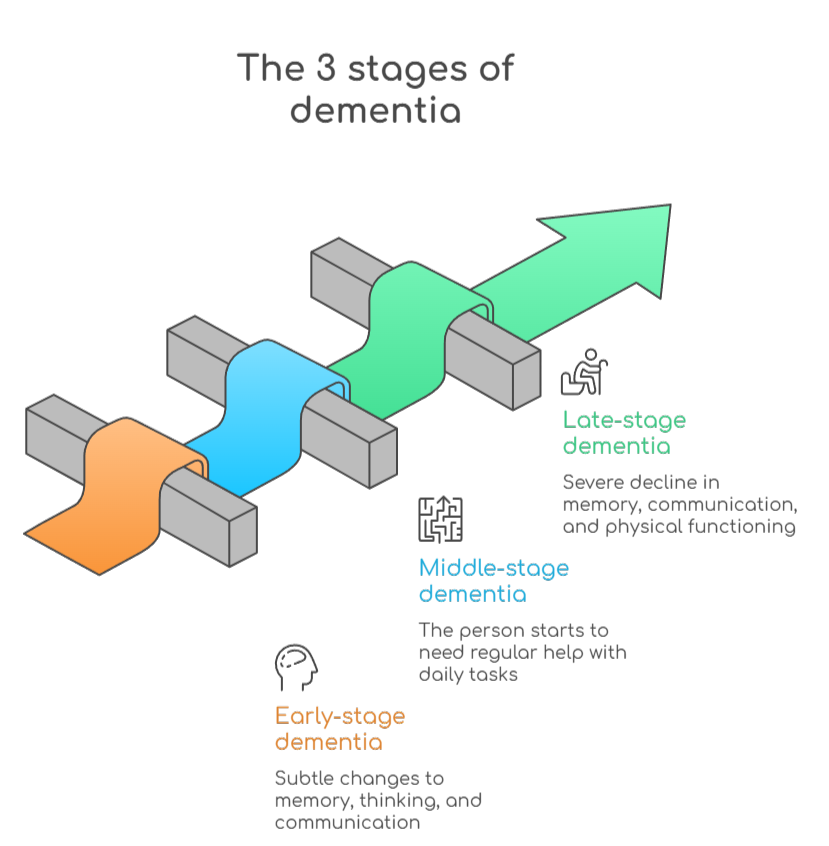
Early-stage dementia (mild)
Early-stage dementia brings subtle changes to memory, thinking, and communication. These changes are noticeable but do not yet stop independent living. The person with dementia may still drive, work, manage their finances, and take part in social activities.
Common signs at this stage include:
- Forgetting recently learned information or recent events, even after being reminded
- Asking the same questions repeatedly within a short time
- Losing track of dates, seasons, or the time
- Struggling to find the right word in conversation
- Difficulty with planning, problem-solving, or following a familiar recipe
- Misplacing items and being unable to retrace steps to find them
- Reduced motivation, increased apathy, or mood changes that seem out of proportion
The person is often aware of their own changes at this stage. This awareness can cause anxiety, low mood, or withdrawal from activities they used to enjoy.
Early-stage dementia is the right time to put legal and financial plans in place. This includes:
- Setting up powers of attorney
- Reviewing wills
- Making decisions about future care while the person still has the legal capacity to do so
Middle-stage dementia (moderate)
Middle-stage dementia is the longest phase of the disease. It lasts between two and ten years, depending on the type of dementia and the person's overall health.
Symptoms become clearly visible to others, and the person starts to need regular help with daily tasks.
During this stage, the person living with dementia may:
- Begin to forget the names of close family members or mix people up
- Become confused about where they are, even in familiar places
- Have significant difficulty with personal hygiene and grooming
- Experience incontinence, first urinary, then bowel
- Show increased agitation, suspicion, or repetitive behaviours
- Wander or try to leave home and become lost
- Sleep at unusual hours or become more confused in the late afternoon (sometimes called "sundowning")
Communication becomes harder. The person uses fewer words, repeats phrases, or struggles to follow a conversation. Judgment is impaired, and daily supervision becomes necessary for safety.
This stage places the greatest strain on family carers. During this stage, important supports include:
- Regular respite care
- Professional home care support
- Carer counselling
Late-stage dementia (severe)
Late-stage dementia involves a severe decline in memory, communication, and physical functioning. The person needs full-time care and cannot be left without support.
Signs of late-stage dementia include:
- Speech reduced to single words, occasional phrases, or no speech at all
- Difficulty swallowing and reduced interest in eating
- Full dependence on carers for bathing, dressing, toileting, and eating
- Loss of ability to walk, then to sit upright without support
- Increased susceptibility to infections, pressure injuries, and falls
- Possible complete loss of recognition of family members
Even in late-stage dementia, the person keeps the ability to feel emotions and respond to touch, familiar voices, and music. Comfort, dignity, and connection remain important until the end of life.
Palliative care becomes the main care focus at this stage, with the goal of maintaining comfort and quality of life. This approach puts symptom relief first, rather than active treatment of the underlying disease.
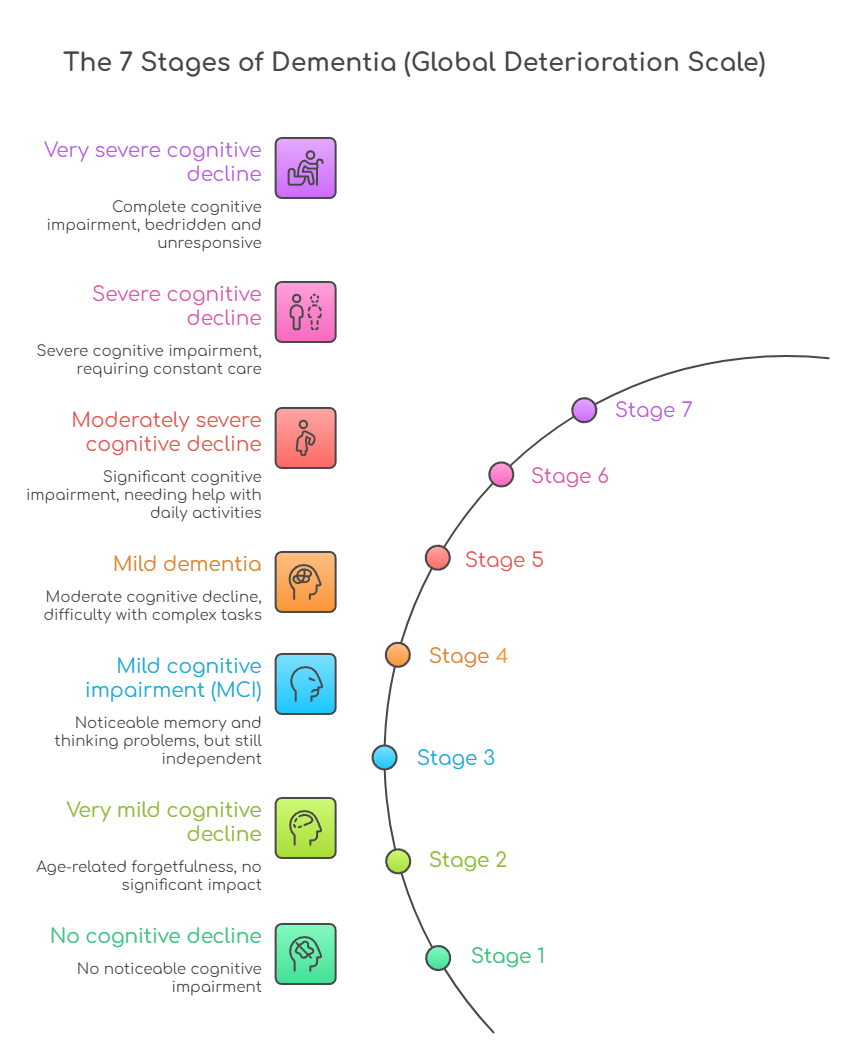
The 7 stages of dementia (Global Deterioration Scale)
The seven-stage GDS model was developed by Dr Barry Reisberg at New York University. Health professionals worldwide use it to track the progression of primary degenerative dementia. It's especially useful for tracking Alzheimer's disease.
Stages 1–3 are pre-dementia stages. Stages 4–7 are the dementia stages.
Stage 1: No cognitive decline
At Stage 1, there are no symptoms and no impairment in memory, thinking, or daily functioning. Brain changes linked to dementia may be silently occurring, but nothing is noticeable.
Stage 2: Very mild cognitive decline (age-related forgetfulness)
At Stage 2, the person may feel they forget names or misplace items more than they used to. These changes are not visible to others or detectable through standard cognitive testing. They are common in adults over 65 and are not, by themselves, a sign of dementia.
Daily life is not significantly affected. However, people at this stage do decline at higher rates than similarly aged adults without these complaints.
Stage 3: Mild cognitive impairment (MCI)
Stage 3 is the earliest point at which changes become noticeable to close family members or colleagues. At this stage, the person:
- May repeat questions
- Struggle to recall recently learned information
- Show reduced performance in complex tasks at work
MCI is not the same as dementia. Daily activities are not yet affected.
In specialist memory clinics, around 10–15% of people with MCI progress to dementia each year. Rates are lower in the general community.
Stage 4: Mild dementia (moderate cognitive decline)
Stage 4 is the first dementia stage on the GDS. Cognitive decline is now evident on clinical assessment, but the person can often still manage basic daily activities.
At this stage, the person may:
- Have difficulty remembering recent events or current affairs
- Struggle to manage finances, plan meals, or organise complex tasks
- Retain long-term memories while short-term memory declines
- Withdraw from family or social situations
- Show early signs of denial about their cognitive changes
Stage 4 corresponds broadly to the early stage in the three-stage model.
Stage 5: Moderately severe cognitive decline
At Stage 5, the person can no longer manage without regular help. Major memory gaps emerge. They may forget personal details such as their own address or phone number, and may not be able to recall the current year.
The person needs help with tasks like choosing appropriate clothing and preparing meals. However, they still remember their own name and recognise close family members.
Stage 5 roughly overlaps with the transition from early to middle dementia in the three-stage model.
Stage 6: Severe cognitive decline
At Stage 6, the person can no longer care for themselves without full daily help. They may forget the names of close family members, confuse a spouse with a parent, or not recognise familiar faces.
The person may also experience:
- Incontinence (urinary first, then bowel)
- Difficulty with basic tasks such as dressing or washing
- Personality changes, delusions, or paranoid beliefs
- Significant agitation, anxiety, or repetitive behaviours
- Disrupted sleep patterns
Speech is still present but may be limited to simple sentences or repetitive phrases.
Stage 7: Very severe cognitive decline
Stage 7 is the final stage of dementia. The person needs full-time care for all activities, including eating, toileting, bathing, and moving.
Speech is gradually lost, starting with a vocabulary of just a few words and eventually reducing to sounds. The brain progressively loses the ability to direct the body. Muscles become rigid.
The person loses the ability to walk, then to sit upright without support, and eventually to swallow safely.
Palliative care is the main focus at this stage, which includes:
- Comfort
- Pain management
- Infection prevention
- Maintaining the person's dignity and connection with family
How long does each stage of dementia last?
Dementia does not follow a fixed timeline. People with the same diagnosis can decline at very different speeds. Doctors cannot accurately predict how quickly one person will move through the stages.
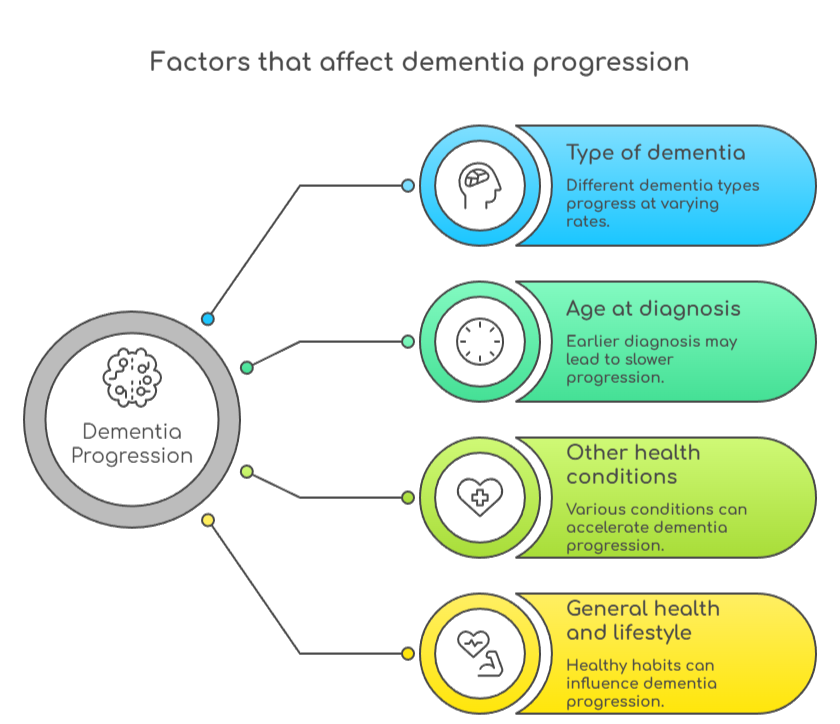
We don't have precise timeframes for each stage. However, we do know roughly how long different types of dementia often last, and which factors affect progression. These factors include:
- The type of dementia
- The age at which the person was diagnosed
- Other health conditions
- General physical health and lifestyle
Type of dementia
Different diseases cause dementia. On average, Alzheimer's disease often lasts about 8–10 years from symptom onset. Lewy body and frontotemporal dementias often progress faster, over roughly 4–8 years.
Age at diagnosis
Younger-onset Alzheimer's (before about 65) often progresses faster than Alzheimer's diagnosed later in life. Older people may decline more slowly, but there are many exceptions.
Other health conditions
Various conditions can speed up decline, especially if they are poorly controlled. For instance, diabetes, heart disease, and high blood pressure. Treating these conditions well can help the person stay as well as possible for longer.
General physical health and lifestyle
Good overall health can support slower progression. Regular physical activity and a balanced diet are linked to better function and fewer complications.
What causes dementia? Understanding the different types
Dementia is caused by different underlying brain diseases. The type affects both the pattern of symptoms and the rate of progression.
Is dementia preventable?
Dementia is not inevitable. Many cases could be prevented or delayed through healthy lifestyle choices.
Staying active is one of the strongest protective factors. Aim for 150–300 minutes of moderate exercise each week, plus strength and balance training twice a week.
Other risk factors you can manage include:
- Uncontrolled high blood pressure, diabetes, and heart disease
- Smoking and heavy drinking
- Untreated hearing loss
- Depression and social isolation
- Head injuries
- Poor diet and obesity
Managing these risk factors does not guarantee prevention. But research consistently shows that reducing them lowers dementia risk across the population.
What about younger people with dementia?
Younger-onset dementia affects people under the age of 65. An estimated 29,000 Australians are living with younger-onset dementia.
Younger people with dementia often face distinct challenges, including:
- Ongoing employment
- Dependent children
- Financial commitments
- Greater awareness of their own decline in the early stages
In Australia, people diagnosed with dementia before age 65 get support through the National Disability Insurance Scheme (NDIS) rather than the aged care system. NDIS funding can cover:
- Help with personal care, such as showering and dressing
- Help with meal preparation, medication management, and domestic tasks
- Transport support
- Allied health services, including speech pathology and dietetics
- Behavioural support planning
- Support to remain connected to work, community, and social activities
Signs it's time to increase support
Dementia progresses gradually, and the right moment to increase support isn't always obvious. Families often wait until a crisis (a fall, a wandering incident, or carer burnout) before making changes. Recognising the signs earlier helps avoid these situations.
Consider increasing support when you notice:
- Safety concerns — wandering, getting lost in familiar places, leaving the stove on, or forgetting to lock doors
- Medication problems — missed doses, double doses, or confusion about what to take and when
- Personal care decline — reduced bathing, wearing the same clothes for days, or noticeable weight loss
- Falls or near-falls — unsteadiness, bruises the person can't explain, or difficulty getting up from chairs
- Incontinence — new or worsening bladder or bowel accidents
- Social withdrawal — avoiding activities they used to enjoy, or appearing confused in conversations
- Carer strain — the main carer feeling exhausted, unwell, or unable to keep up with demands
Any one of these signs is worth acting on. Together, they often signal that the current level of support is no longer enough.
Speaking with a GP, dementia nurse, or home care provider early can help you plan the next step. This might mean introducing in-home help, arranging respite care, or reviewing medication and safety at home.
Dementia stages and care planning: what support is needed at each stage?
The level of support a person needs changes greatly as dementia progresses. Planning ahead at each stage prevents crisis situations. It also helps the person with dementia stay in their preferred environment for as long as possible.
In-home care is available and appropriate across all three stages. But the hours and type of support needed grow significantly through the middle and late stages. Many families use a mix of family care and funded in-home support services, particularly in the middle stage.
FAQ
What is the difference between dementia stages and normal ageing?
Normal ageing involves occasional memory lapses that don't significantly affect daily life. For example, briefly forgetting a name before recalling it. Dementia is different. It causes progressive decline in memory, language, and judgment that is severe enough to interfere with daily life. Dementia is not a normal part of ageing.
How long does the final stage of dementia last?
How long late-stage dementia lasts varies greatly between individuals. It also depends on the type of dementia, the person's age, and their overall physical health. It is not possible to predict how long any individual will remain in the final stage.
Can dementia be reversed?
No. For the most common types of dementia, damage to brain cells cannot be reversed. A newer treatment, Leqembi (lecanemab), was approved in Australia in September 2025. It can slow the decline in early Alzheimer's disease for eligible patients. It does not reverse existing cognitive loss, and eligibility depends on genetic testing and disease stage.
Some conditions that look like dementia are treatable. This includes vitamin B12 deficiency, hypothyroidism, or medication side effects. This is why a thorough medical assessment is important when cognitive changes first appear.
Is dementia the same as Alzheimer's disease?
No. Dementia is the umbrella term for a group of symptoms caused by different underlying brain diseases. Alzheimer's disease is the most common cause, accounting for 60%–80%of cases (National Institute on Aging). Other types include vascular dementia, Lewy body dementia, and frontotemporal dementia.
How Sensible Care supports people living with dementia
Sensible Care provides government-funded in-home dementia care. Services are available under Support at Home, NDIS, CHSP, DVA, and six other funding types. You can access support regardless of which programme funds you. There are no lock-in contracts, no daily fees, and no exit charges.
Sensible Care's in-house allied health team includes physiotherapists, occupational therapists, podiatrists, and dietitians. Community nursing is delivered by qualified nurses at home.
We also handle all the paperwork and provider-switching administration on your behalf, so you can focus on your loved one. Book a free initial consultation by phone or schedule a callback to get started.
Take the Next Step in Care
Download our Info Kit or speak to one of our friendly team members today.
Need Help Getting Started?
Reach out on your terms, pick a time that suits you and let’s talk about how we can help.
.webp)
.svg)


